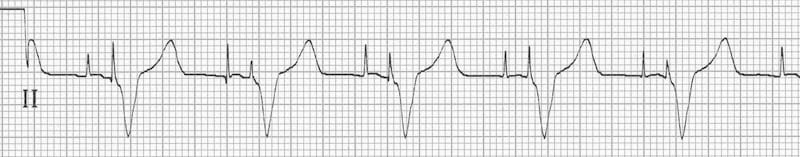 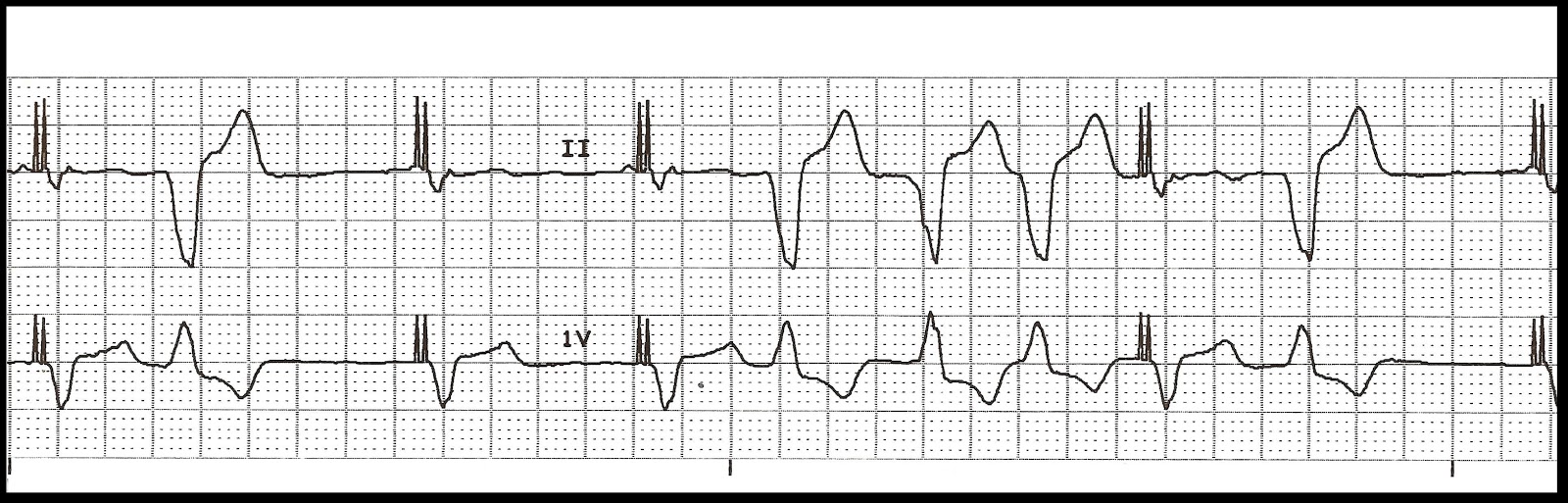
The details of these studies will be shown in the following sections respectively. Since the implementation of specific algorithms for avoidance of unnecessary RV stimulation in modern PM and ICD systems several studies have shown the clinical relevance and necessity of this approach. It was therefore speculated that the risk of HFH in the DDDR mode would not increase with further increases in cum%RVP above 40%, but a further risk reduction to about 2% could be achieved with minimization of unnecessary RV pacing (VP 2% is an independent predictor for the occurrence of ventricular tachyarrhythmias, mortality and episodes of heart failure in ICD patients (who had predominantly secondary prophylactic ICD indications). Patients with an ejection fraction 40% in the DDDR mode. The original intention of the DAVID trial (Dual Chamber and VVI Implantable Defibrillator) was to show a survival benefit of dual chamber ICD systems compared to single chamber ICDs. The first evidence for clinically relevant negative effects of a high percentage of RV pacing was found interestingly in studies that were originally intended to show benefits of “physiologic” AV sequential DDD stimulation compared to VVI stimulation. Clinical consequences of unnecessary right ventricular pacing The delayed dyssynchronous activation of the ventricles with RV stimulation is visible in the ECG by a more or less deformed and widened QRS complex ( Fig. This late systolic contraction delays the passive ventricular filling and thereby shortens the effective duration of diastole ( Fig. Whereas the first activated areas of myocardium already enter the relaxation cycle, the delayed activated ones can still be in systolic contraction. The electromechanical dyssynchrony influences the diastole as well. Transmitral Doppler shows fusion of E- and A-wave, representing an overlap of the passive and active LV filling, which is therefore shortened and reduced. 2a) is longer than Δt 2: from the beginning of the QRS complex to the start of transmitral filling ( fig. The time interval Δt 1 from the beginning of the QRS complex to the end of anterior movement of the LV-PLW ( fig. Demonstration of systolic contraction of the left posterolateral ventricular wall (LV-PLW) while there is already left ventricular filling. TTE, m-mode, parasternal long axis (PLAX) 2b. In the ejection phase the early activated areas will be able to contract only a little further, whereas the later activated areas will contract 1) delayed and 2) increased due to the previous stretching ( Fig. The dyssychronous contraction resulting from atypical excitation due to pacing can be compared to the situation in patients with conduction delay or block in the left Tawara-bundle (left bundle branch block (LBBB)).Īt the start of systole (isovolumetric phase) the myocardial fibers near the RVA-pacing site will be the first ones to shorten, whereas the more remote left lateral ventricular areas will go into passive stretching, as they are lacking electrical excitation at this point. The exact individual sequence of excitation and contraction will be influenced by stimulus location, activation of parts of the specific conduction system and electroanatomical characteristics of the myocardium (fibrosis, scars). For example, the conduction after stimulation in the RV apex (RVA) will occur mostly in the working myocardium with a significantly lower velocity ≤1 m/s in an apico-basal direction from the RV via the interventricular septum to the left ventricle (LV). Similar to the excitation in a premature ventricular contraction (PVC) or following conduction through an antegrade conducting bypass tract, ectopic ventricular stimulation will result in a more or less non-physiologic activation and therefore non-physiologic contraction sequence of the ventricles. This is the basis for an optimum hemodynamic contraction sequence in all heart chambers. With intact cardiac conduction, the physiological excitation of the ventricles occurs with high velocity (3-4m/s) via the His‐Purkinje‐system (HPS) nearly synchronously. Pathophysiology of right ventricular stimulation
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
